The video posted to our Youtube Channel is NOT sponsored and Youtube Advertising deems storm chasing and natural disaster videos as not advertiser …
Perspectives and the Demand for Digital Health Innovations During a Pandemic
Expert panel representing industry, healthcare providers and patients. Moderated by Dr. Nassir F. Marrouche, Chair, HRS Digital Health Committee and …
Life Insurance Companies Are Doing The "Unthinkable" – Turning Away Life Insurance
Life Insurance Companies Are Doing The “Unthinkable” – Turning Away Life Insurance 0:23 – Life insurance can be an important part of financial planning 1:51 …
SR22 Auto Insurance Quotes — Illinois, Florida, Tennessee
SR22 Auto Insurance Quotes — Illinois, Florida, Tennessee Related topics: sr22 auto insurance, sr22 auto insurance quotes, usaa sr22 auto insurance, low cost …
Subsidy availability drives consumers to shop for health insurance
A major premise of the Affordable Care Act (ACA) was that Americans who need to buy their own health coverage in the individual market should be able to obtain coverage – regardless of their medical history – and that the monthly premiums should be affordable.
The rules to facilitate those goals have been in place for several years now. And although they have worked quite well for some Americans, there have been others for whom ACA-compliant health coverage was still unaffordable.
But the American Rescue Plan, enacted earlier this year, has boosted the ACA’s subsidies, making truly affordable coverage much more available than it used to be.
The numbers speak for themselves: Exchange enrollment has likely reached a record high of nearly 13 million people in 2021, after more than 2.5 million people enrolled during the COVID/American Rescue Plan enrollment window, which ended this month in most states.
How much are consumers saving on health insurance premiums?
And the amount that people are paying for their coverage and care is quite a bit lower than it was before the APR’s subsidy enhancements. We can see this across the states that use the federally run exchange (HealthCare.gov), as well as the states that run their own exchanges:
- Among the people who enrolled during the recent special enrollment period in the 36 states that use HealthCare.gov, average after-subsidy premiums were 27% lower than the amounts people were paying pre-ARP.
- Among HealthCare.gov enrollees who signed up during the special enrollment period or who updated their enrollments to claim the enhanced subsidies, 35% are now paying less than $10/month for their coverage.
- Average deductibles for new HealthCare.gov enrollees were 90% lower than pre-ARP deductibles, likely driven in large part by the number of people who were able to enroll in free or low-cost Silver plans with built-in cost-sharing reductions. (This includes people receiving unemployment compensation in 2021, as well as people who aren’t eligible for Medicaid and whose household income is between 100% and 150% of the federal poverty level.)
- The state-run exchange in Washington reported that 78% of their enrollees are now receiving premium subsidies, versus 61% before the ARP was implemented. And consumers with income above 400% of the poverty level, who were not eligible for subsidies pre-ARP, are now paying an average of $200 less in premiums each month. Washington’s exchange also noted that 15% of their enrollees are now paying $1/month or less for their coverage, versus only 5% whose premiums were that low pre-ARP.
- The state-run exchange in California reported that consumers with household incomes between 400% and 600% of the poverty level are saving an average of almost $800/month on their premiums. (That’s an individual with income up to about $76,000, or a household of four with an income up to about $157,000.)
- The state-run exchange in Nevada reported that people who enrolled or updated their account since the ARP was implemented are paying an average of $154/month in after-subsidy premiums, whereas the after after-subsidy premium at the end of last winter’s open enrollment period (pre-ARP) was $232/month.
- Maryland’s state-run exchange reported a 12% increase in the number of enrollees receiving subsidies; more than 80% of Maryland’s current exchange enrollees are subsidy-eligible.
These examples highlight the improved affordability that the ARP has brought to the health insurance marketplaces. People who were already eligible for subsidies are now eligible for larger subsidies. And many of the people who were previously ineligible for subsidies — but potentially facing very unaffordable health insurance premiums — are benefiting from the ARP’s elimination of the income cap for subsidy eligibility.
How long will the ARP’s subsidy boost last?
Although the ARP’s subsidies for people receiving unemployment compensation in 2021 are only available until the end of this year, the rest of the ARP’s premium subsidy enhancements will continue to be available throughout 2022 — and perhaps longer, if Congress extends them.
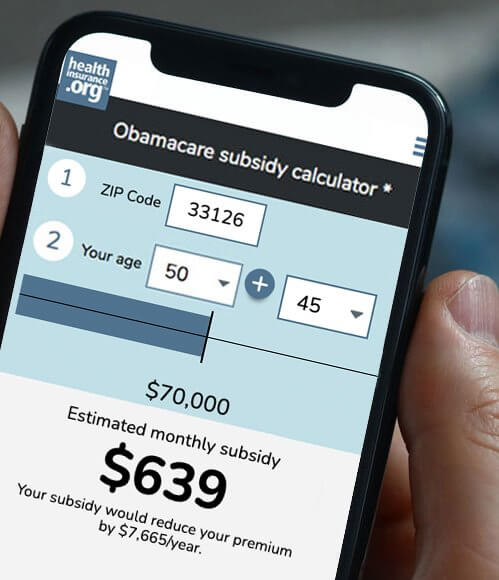
Use our updated subsidy calculator to estimate how much you can save on your 2021 health insurance premiums.
This means that the affordability gains we’ve seen this year will be available during the upcoming open enrollment period, when people are comparing their plan options for 2022.
Robust ACA-compliant coverage will continue to be a more realistic option for more people, reducing the need for alternative coverage options such as short-term plans, fixed indemnity plans, and health care sharing ministry plans.
Even catastrophic plans – which are ACA-compliant but not compatible with premium subsidies – are likely to see reduced enrollment over the next year, since more people are eligible for enhanced subsidies that make metal-level plans more affordable.
Can everyone find affordable health insurance now?
Unfortunately, not yet. There are still affordability challenges facing some Americans who need to obtain their own health coverage. That includes more than two million people caught in the “coverage gap” in 11 states that have refused to expand eligibility for Medicaid, as well as about 5 million people affected by the ACA’s “family glitch.”
There are strategies for avoiding the coverage gap if you’re in a state that hasn’t expanded Medicaid, and Congressional lawmakers are also considering the possibility of a federally-run health program to cover people in the coverage gap.
Families affected by the family glitch have access to an employer-sponsored plan that’s affordable for the employee but not for the whole family – and yet the family is also ineligible for subsidies in the marketplace/exchange. (It’s possible that the Biden administration could tackle this issue administratively in future rulemaking.)
Have ARP’s subsidy boosts been successful?
With the exception of those two obstacles, the ARP has succeeded in making affordable health coverage a more realistic option for most Americans who need to obtain their own health coverage. We can see success in the record-high exchange enrollment, the increased percentage of enrollees who are subsidy-eligible, and the reduction in after-subsidy premiums that people are paying.
If you’re currently uninsured or covered by a non-ACA-compliant plan (including a grandfathered or grandmothered plan), it’s in your best interest to take a moment to see what your options are in the ACA-compliant market. Open enrollment for 2022 coverage starts in just two months, but you may also find that you can still enroll in a plan for the rest of 2021 if you live in a state where a COVID/American Rescue Plan enrollment window is ongoing, or if you’ve experienced a qualifying event recently (examples include loss of employer-sponsored insurance, marriage, or the birth or adoption of a child).
Even if you shopped just last winter, during open enrollment for 2021 plans, you might be surprised at the difference between the premiums you would have paid then and now. The ARP wasn’t yet in effect during the last open enrollment period, so if you weren’t eligible for a subsidy last time you looked, or if the plans still seemed too expensive even with a subsidy, you’ll want to check again this fall.
The subsidies for 2022 will continue to be larger and more widely available than they’ve been in the past, and you owe it to yourself to see what’s available in your area.
Louise Norris is an individual health insurance broker who has been writing about health insurance and health reform since 2006. She has written dozens of opinions and educational pieces about the Affordable Care Act for healthinsurance.org. Her state health exchange updates are regularly cited by media who cover health reform and by other health insurance experts.
twenty one pilots: Car Radio [OFFICIAL VIDEO]
twenty one pilots’ music video for ‘Car Radio’ from the album, Vessel – available now on Fueled By Ramen. http://smarturl.it/vessel Download/Stream their new …
Who Buys Private Health Insurance? – RES 2014
Who pays for private health insurance? In what way are they different? RES Prize winners Pau Olivella (Barcelona Graduate School of Economics and …
Your Life Insurance Sucks!
Did you miss the latest Ramsey Show episode? Don’t worry—we’ve got you covered! Get all the highlights you missed plus some of the best moments from the …
Auto insurance quotes online
compare car insurance,car insurance compare,compare insurance quotes,ompare health insurance,compare home insurance. compare car insurance quotes …
Congress boosted ACA subsidies. An enrollment surge followed.
The American Rescue Plan, signed into law by President Biden on March 11 of this year, included major boosts to the affordability of health plans sold in the ACA marketplace for people of all incomes.
Effective through 2022 and likely to be made permanent by pending legislation, the ARP improvements to affordability were as follows:
- A benchmark Silver plan (the second least expensive Silver plan) with strong cost sharing reduction (CSR) subsidies became free to enrollees with household income up to 150% of the Federal Poverty Level (FPL) and costs no more than 2% of income for enrollees with income up to 200% FPL. That’s a maximum of $43 per month for a single person with an income of $25,520.
- The previous income cap on subsidy eligibility was removed, so that no one who lacks access to affordable coverage elsewhere (i.e., from an employer) has to pay more than 8.5% of income for a benchmark Silver plan (less at lower incomes). The eliminated cap was 400% FPL ($51,040 for an individual, $104,880 for a family of four), and some households with income well above that level now qualify for subsidies.
- The percentage of income required to buy a benchmark Silver plan was reduced at all income levels.
- Anyone who received any unemployment insurance income during 2021 was eligible for free high-CSR Silver coverage. (Note that the pending legislation calls for this subsidy enhancement to be extended by several years, but not necessarily made permanent.)

Our 2022 Open Enrollment Guide: Everything you need to know to enroll in an affordable individual-market health plan.
Preceding and then coinciding with these major subsidy boosts, the Biden administration had opened an emergency Special Enrollment Period (SEP) running from February 15 through August 15 in the 36 states that use the federal ACA exchange, HealthCare.gov.
The SEP, implemented to help Americans get covered during the pandemic, functioned like a second open enrollment period: anyone who lacked access to affordable coverage from other sources (e.g., employers) could enroll in a marketplace plan. The 15 state-based exchanges also opened emergency SEPs, with somewhat different durations and conditions, summarized here.
ARP prompted an enrollment surge during the 2021 SEP
The enhanced subsidies were posted on HealthCare.gov on April 1, and in the state-run exchanges within a few weeks of that date. Existing enrollees were encouraged to update their information and get the new subsidies credited, and were allowed to switch plans if they chose.
Americans responded with a major surge in new enrollment and enrollment upgrades. From February 15 through August 15:
- More than 2.8 million people enrolled in new health coverage. Of new enrollees, 91% qualified for premium subsidies.
- Of new enrollees, 44% obtained coverage for less than $10 per month. Most of these enrollees (41% in HealthCare.gov states) received free coverage with the highest level of CSR. As a result, the median deductible fell from $750 in 2020 to $50 this year – meaning that half of enrollees obtained a plan with a deductible at or below that level (most of them in high-CSR Silver plans).
- The average premium paid by new consumers during the SEP (Feb. 15 – Aug. 15) fell 30%, from $117 in 2020 to $81 in 2021.
- Marketplace enrollment in August 2021, at 12.2 million, was 15% higher than in August 2020, the previous August high, and 22% above the pre-pandemic August high (see p. 14 here) recorded in 2016.
- More than 200,000 new and existing enrollees qualified for free high-CSR Silver plans because they had received unemployment insurance income in 2021.
Savings were also dramatic for existing marketplace enrollees:
- 8 million existing enrollees reduced the premiums on their existing plans or obtained new plans after ARP implementation.
- Existing enrollees reduced their premiums by 50%, or by $67 per month, on average.
My premium went down how much?
To get a sense of the extent to which the ARP reduced enrollee costs (or encouraged people who might previously have considered coverage too expensive to enroll), consider these examples:
- In November 2020, a 40-year-old in Miami with an income of $24,000 per year would have paid $115 per month for the least expensive available Silver plan, with a $1,500 deductible, and $119 per month for the second-cheapest Silver plan, with a $0 deductible. Thanks to the ARP, those plans would now cost this person $26 and $30 per month, respectively.
- In November 2020, a pair of 60-year-olds in Dallas, Texas with an income of $70,000 – slightly over the income cap for premium subsidies, which the ARP eliminated – would have had to pay $1,669 per month for the lowest cost Gold plan, with a $2,300 deductible (Gold plans are cheaper than Silver Plans in Dallas), or $1,228 for the lowest cost Bronze plan, with an $8,550 deductible.
Now, this couple can choose to pay $393 per month for the Gold plan (which includes free doctor visits and generic drug prescriptions, neither subject to the deductible), or consider two free Bronze plans with deductibles over $8,000, a $2/month Bronze plan with a $6,100 deductible, and other options. A BlueCross Silver plan available for $420 per month might also be in the mix, if, say, the provider network is preferable.
Which states saw the biggest gains in new enrollees?
The new enrollment surge – and the savings – was particularly strong in twelve states that had not enacted the ACA Medicaid expansion as of June 2021. Due to their failure to expand Medicaid, these states have a “coverage gap” for people who earn too little to qualify for marketplace coverage (less than 100% FPL, or $12,760 for an individual in 2021) but mostly also don’t qualify for Medicaid because of their states’ restrictive Medicaid eligibility. (That excludes Wisconsin, which has not enacted the ACA expansion but grants Medicaid eligibility to adults with income up to 100% FPL. Oklahoma, which expanded Medicaid beginning in July 2021, and Missouri, which will begin covering new Medicaid expansion enrollees in October, are included.)
These twelve states – Alabama, Florida, Georgia, Kansas, Missouri, Mississippi, North Carolina, Oklahoma, South Carolina, South Dakota, Tennessee, Texas and Wyoming – accounted for 1.55 million new enrollees during the SEP, or 55% of all new enrollees nationally.
In the non-expansion states, eligibility for marketplace subsidies begins at 100% FPL, as opposed to 138% FPL in Medicaid expansion states, where adults below that threshold qualify for Medicaid. Accordingly, in these states, about half of enrollees qualified for free high-CSR coverage, reporting incomes between 100% and 150% FPL. In these states, enrollment as of August 2021 (6.0 million) was 44% above enrollment in August 2019, the last pre-pandemic year (4.2 million).
More than 2 million people in non-expansion states are estimated to be stuck in the coverage gap – ineligible both for Medicaid and for ACA premium subsidies. For people in these states, reporting an income just below or just above 100% FPL ($12,760 for an individual, $26,200 for a family of four) is the difference between receiving no help at all and having access to free Silver coverage with high CSR and low out-of-pocket costs.
It’s important to keep in mind that the application for marketplace coverage requires an income estimate – and many people, unaware of the minimum income requirement, underestimate their potential income. For tips on how to make sure you leave no stone unturned in seeking help paying for coverage, see this post.
What do these numbers mean for 2022 open enrollment?
As open enrollment for 2022 approaches (it begins on November 1), the subsidies enhanced by the ARP remain in place for 2022. As Congress hashes out new investments for coming years in a pending budget bill, the pressure is intense to keep this good thing going in future years.
As of now, with the sad exception of those stuck in the coverage gap in states that still refuse to enact the ACA Medicaid expansion, any citizen or legally present noncitizen who lacks access to other forms of affordable coverage should be able to find it in the marketplace. If you need coverage, make sure to check out your options on HealthCare.gov or your state exchange.
The word that ACA marketplace plans are more affordable than ever has not yet reached many of the people who need coverage and qualify for premium subsidies. The Kaiser Family Foundation estimated in May that nearly 11 million uninsured people were subsidy-eligible. ACA enrollment assisters consistently report that many people who are eligible for coverage have no idea what’s on offer.
The Biden administration is trying to change that: after years of radical cuts in federal funds for enrollment assistance, the administration this year has allocated a record $80 million to fund nonprofit enrollment “navigator” groups charged with outreach as well as enrollment assistance. The Urban Institute forecast that if the ARP subsidies are made permanent – solidifying the perception that truly affordable coverage is here to stay — enrollment would increase by more than 5 million in 2022.
The emergency SEP provided a jump start, boosting coverage as of August more than 1.5 million above the August 2020 level. In a fraught and complex legislative session, Congress will most likely – though not certainly – do its part and extend the subsidies beyond 2022. There is certainly room for enrollment to run higher in the open enrollment season that begins on November 1.
Andrew Sprung is a freelance writer who blogs about politics and healthcare policy at xpostfactoid. His articles about the Affordable Care Act have appeared in publications including The American Prospect, Health Affairs, The Atlantic, and The New Republic. He is the winner of the National Institute of Health Care Management’s 2016 Digital Media Award. He holds a Ph.D. in English literature from the University of Rochester.
Ash Cash On Investing In Bitcoin, Differences In Life Insurance, Savings & Investment Accounts
Ash Cash the financial Guru gives tips on saving and investing money, especially during the pandemic. Subscribe Here! http://bit.ly/SubscribeSU Watch the Best …
Top 7 Reasons of Rejection of Motor Insurance Claim
This video helps you to understand the top reason due to which most of the motor claim got rejected, it does not matter how broad coverage you have taken …
Biden Delivers Remarks On Health Care | NBC News
Watch live coverage as former Vice President Joe Biden delivers remarks on health care and the Affordable Care Act. » Subscribe to NBC News: …
Think you’re not eligible for ACA subsidies? Think again.
For millions of Americans, the open enrollment period (OEP) to shop for 2022 ACA-compliant coverage will be unlike any of the previous eight OEPs. The reason? These consumers will – for the first time – be able to tap into the Affordable Care Act’s premium tax credits (more commonly referred to as health insurance subsidies).
Thanks to the American Rescue Plan, consumers who in previous years might have found themselves outside the eligible level for subsidies – or who may have found that subsidy amounts were so low as to not be enticing – are now among those eligible for premium tax credits. So if you haven’t shopped for health insurance lately, you might be surprised to see how affordable your health coverage options are this fall (starting November 1), and how many plan options are available in your area.
Millions have already tapped into the subsidies
Most people who currently have coverage through the health insurance exchanges have seen improved affordability this year thanks to the American Rescue Plan (ARP). That includes millions of people who were already enrolled in plans when the ARP was enacted last March, as well as millions of others who signed up during the special enrollment period that continued through mid-August in most states (and is still ongoing in some states).
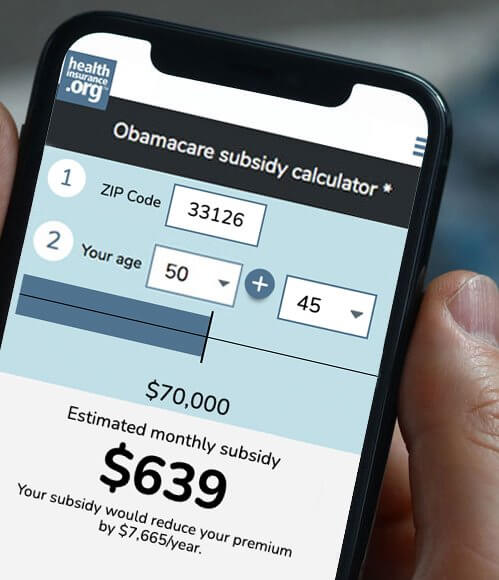
Use our updated subsidy calculator to estimate how much you can save on your 2021 health insurance premiums.
But there are still millions of others who are either uninsured or have obtained coverage elsewhere. And there are also people who already had coverage in the exchange in 2021 but didn’t take the option to switch to a more robust plan after the ARP was implemented. If you’re in either of these categories, you don’t want to miss the open enrollment period in the fall of 2021.
The Build Back Better Act, which is still under consideration in Congress, would extend the ARP’s subsidies and ensure that health insurance stays affordable in 2023 and beyond. But even without any new legislative action, most of the ARP’s subsidy enhancements will remain in place for 2022.
That means there will continue to be no upper income limit for premium tax credit (subsidy) eligibility, and the percentage of income that people have to pay for the benchmark plan will continue to be lower than it was in prior years. The overall result is that subsidies are larger than they were in the past, and available to more people.
Who should make a point to review their subsidy eligibility?
So who needs to pay close attention this fall, during open enrollment? In reality, anyone who doesn’t have access to Medicare, Medicaid, or an employer-sponsored health plan – because even if you’re already enrolled and happy with the plan you have, auto-renewal is not in your best interest.
But there are several groups of people who really need to shop for coverage this fall. Let’s take a look at what each of these groups can expect, and why you shouldn’t let open enrollment pass you by if you’re in one of these categories:
1. The uninsured – eligible for low-cost or NO-cost coverage
The majority of uninsured Americans cite the cost of coverage as the reason they don’t have health insurance. Yet millions of those individuals are eligible for free or very low-cost health coverage but haven’t yet enrolled. This has been the case in prior years as well, but premium-free or very low-cost health plans are even more widely available as a result of the ARP.
If you’re uninsured because you don’t think health insurance is affordable, know that more than a third of the people who enrolled via HealthCare.gov during the COVID/ARP special enrollment period this year purchased plans for less than $10/month.
Even if you’ve checked in previous years and couldn’t afford the plans that were available, you’ll want to check again this fall, since the subsidy rules have changed since last year.
2. Consumers enrolled in non-ACA-compliant plans
There are millions of Americans who have purchased health coverage that isn’t compliant with the ACA. Most of these plans are either less robust than ACA-compliant plans, or use medical underwriting, or both. They include:
People purchase or keep these plans for a variety of reasons. But chief among them has long been the fact that ACA-compliant coverage was unaffordable – or was assumed to be unaffordable.
There are also people who prefer some of the benefits that some of these plans offer (the fellowship of being part of a health care sharing ministry, for instance, or the abundantly available primary care with a DPC membership). But by and large, the reason people choose coverage that isn’t ACA-compliant, or that isn’t even insurance at all, is because ACA-compliant coverage doesn’t fit in their budgets.
This has long included a few main groups of people: Those who earned too much to qualify for subsidies, those affected by the “family glitch,” and those who qualified for only minimal subsidy assistance and still felt that the coverage available in the exchange wasn’t affordable.
(Another group of people unable to afford coverage are those who earn less than the poverty level in 11 states that have refused to expand Medicaid and thus have a coverage gap. Some people in the coverage gap purchase non-ACA-compliant coverage, but this population is also likely to not have any coverage at all. If you or a loved one are in the coverage gap, we encourage you to read this article.)
The ARP has not fixed the family glitch or the coverage gap, although there are legislative and administrative solutions under consideration for each of these.
But the ARP has addressed the other two issues, and those provisions remain in place for 2022. The income cap for subsidy eligibility has been eliminated, which means that some applicants can qualify for subsidies with income far above 400% of the poverty level. And for those who were already eligible for subsidies, the subsidy amounts are larger than they used to be, making coverage more affordable.
So if you are enrolled in any sort of self-purchased health plan that isn’t compliant with the ACA, you owe it to yourself to check your on-exchange options this fall, during the open enrollment period. Keep in mind that you can do that through the exchange, through an enhanced direct enrollment entity, or with the assistance of a health insurance broker.
3. Buyers enrolled in off-exchange health plans
There are also people who have “off-exchange” ACA-compliant plans that they’ve purchased directly from an insurance company, without using the exchange. (Note that this is not the same thing as enrolling in an on-exchange plans through an enhanced direct enrollment entity, many of which are insurance companies).
There are a variety of reasons people have chosen to enroll in off-exchange health plans over the last several years. And for some of those enrollees, 2022 might be the year to switch to an on-exchange plan.
Since 2018, some people have opted for off-exchange plans if they weren’t eligible for premium subsidies and wanted to enroll in a Silver-level plan. This was a very rational choice, encouraged by state insurance commissioners and marketplaces alike. But if you’ve been buying off-exchange coverage in order to get a Silver plan with a lower price tag, the primary point to keep in mind for 2022 is that you might find that you’re now eligible for premium subsidies.
Just like the people described above, who have enrolled in various non-ACA-compliant plans in an effort to obtain affordable coverage, the elimination of the income limit for subsidy eligibility is a game changer for people who were buying off-exchange coverage to get a lower price on a Silver plan.
Some people have opted for off-exchange coverage because their preferred health insurer wasn’t participating in the exchange in their area. This might have been a deciding factor for an applicant who was only eligible for a very small subsidy — or no subsidy at all — and was willing to pay full price for an off-exchange plan from the insurer of their choice.
But 2022 is the fourth year in a row with increasing insurer participation in the exchanges, and some big-name insurers are joining or rejoining the exchanges in quite a few states. So if you haven’t checked your on-exchange options in a while, this fall is definitely the time to do so. You might be surprised to see how many options you have, and again, how affordable they are.
4. Consumers enrolled in on-exchange plans, but no income details on file and no recent coverage reconsiderations
If you’re already enrolled in an on-exchange plan and you had given the exchange a projection of your income for 2021, you probably saw your subsidy amount increase at some point this year.
But if the exchange didn’t have an income on file for you, they wouldn’t have been able to activate a subsidy on your behalf (on the HealthCare.gov platform, subsidy amounts were automatically updated in September for people who hadn’t updated their accounts by that point, but only if you had provided a projected income to the exchange when you enrolled in coverage for 2021). And even if your subsidy amount did get updated, you might have remained on the plan you had picked last fall, despite the option to pick a different one after the ARP was enacted.
The good news is that you’ll be able to claim your full premium tax credit, for the entirety of 2021, when you file your 2021 tax return (assuming you had on-exchange health coverage throughout the year). And during the open enrollment period for 2022 coverage, you can provide income information to the exchange so that a subsidy is paid on your behalf each month next year.
Reconsidering your plan choice during open enrollment might end up being beneficial as well. If you didn’t qualify for a subsidy in the past, or if you only qualified for a modest subsidy, you might have picked a Bronze plan or even a catastrophic plan, in an effort to keep your monthly premiums affordable.
But with the ARP in place, you might find that you can afford a more robust health plan. And if your income doesn’t exceed 250% of the poverty level (and especially if it doesn’t exceed 200% of the poverty level), pay close attention to the available Silver plans. The larger subsidies may make it possible for you to afford a Silver plan with built-in cost-sharing reductions that significantly reduce out-of-pocket costs.
One other point to keep in mind: If you are receiving a premium subsidy this year, be aware that it might change next year due to a new insurer entering the market in your area and offering lower-priced plans. Here’s more about how this works, and what to consider as you’re shopping for coverage this fall.
The takeaway point here? Even if you’ve been happy with your plan, you should check your options during open enrollment. This is not the year to let your plan auto-renew. Be sure you’ve provided the exchange with an updated income projection for 2022, and actively compare the plans that are available to you. It’s possible that a plan with better coverage or a broader provider network might be affordable to you for 2022, even if it was financially out of reach when you checked last fall.
Louise Norris is an individual health insurance broker who has been writing about health insurance and health reform since 2006. She has written dozens of opinions and educational pieces about the Affordable Care Act for healthinsurance.org. Her state health exchange updates are regularly cited by media who cover health reform and by other health insurance experts.
Taxi Car Garage | Halloween Car Video For Preschool Kids By Kids Channel
Hi Kids! Watch this Taxi Car Garage for children by Kids Channel! We hope you enjoy watching this cartoon for toddlers as much as the Kids Channel team did …



![twenty one pilots: Car Radio [OFFICIAL VIDEO] twenty one pilots: Car Radio [OFFICIAL VIDEO]](https://bestinsurancecenter.com/wp-content/uploads/2022/01/1641862686_maxresdefault-768x432.jpg)