In 2013 the Hospital Readmissions Reduction Program (HRRP), an initiative of the Affordable Care Act (ACA), authorized the Centers for Medicare and Medicaid Services (CMS) to penalize hospitals for thirty-day readmission rates exceeding the national average.
Safety-net hospital patients, who frequently lack access to primary care and other support, have a higher chance of readmission. As a result, policy makers have called for modifications in the HRRP to remove a perceived unfair burden on safety-net hospitals.
A new Health Affairs study, Hospital Readmissions Reduction Program: Safety-Net Hospitals Show Improvement, Modifications To Penalty Formula Still Needed, by Kathleen Carey and Meng-Yun Lin, compared thirty-day readmission rates of safety-net hospitals and other hospitals for fiscal years 2013 and 2016. Three conditions were evaluated: heart attack, heart failure, and pneumonia.
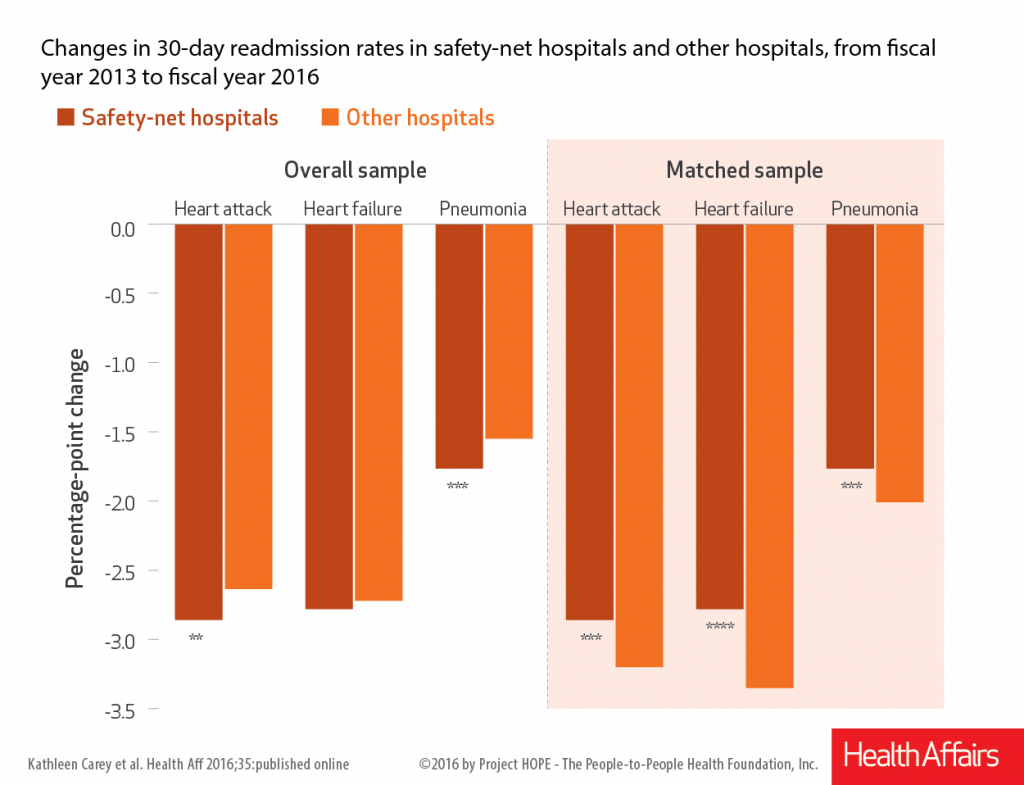
According to the study, readmission rates during that time declined more at safety-net hospitals than at other hospitals in the overall sample for each condition (see exhibit), with heart attack readmissions declining 2.86 percentage points at safety-net hospitals, compared to 2.64 percentage points at other hospitals.
The authors, who obtained their data from Medicare’s Hospital Compare website, note that while safety-net hospitals’ thirty-day readmission rates have declined at a higher rate than other hospitals, the former group had greater room for improvement.
“In refining the HRRP, policy makers should bear in mind that a penalty program may not provide the best lever for incentivizing performance improvement in safety-net hospitals,” the authors concluded. “It would be advisable for CMS to pay attention to characteristics of hospitals that succeed in reducing readmissions as it modifies and expands the HRRP.”